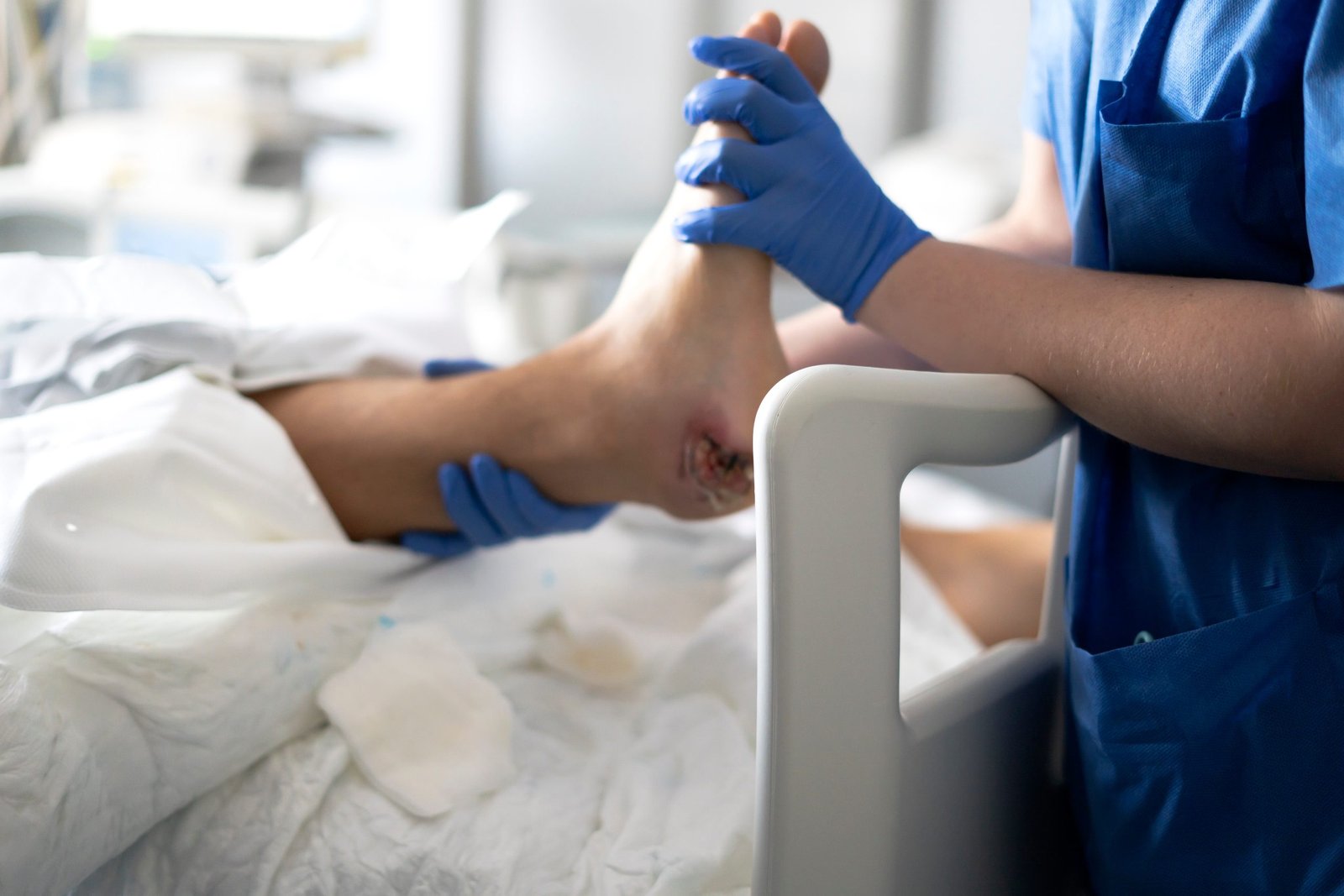
Home Rehabilitation Programs
Home rehabilitation programs have become an essential part of recovery for patients with limited mobility. Conditions such as stroke, fractures, post-surgical recovery, neurological disorders, and age-related weakness often require long-term rehabilitation at home. While home-based therapy offers comfort, convenience, and family support, certain complications can significantly slow down recovery if not addressed in time.
One such commonly overlooked but serious complication is bedsores, also known as pressure ulcers. These wounds can delay rehabilitation, increase pain, and reduce a patient’s ability to actively participate in therapy. Understanding their impact and management is crucial for successful home rehabilitation.
What Are Bed Sores?
Bedsores are areas of skin and underlying tissue damage caused by prolonged pressure, friction, or shear forces. They usually develop when a person remains in one position for too long without adequate movement or pressure relief.
Common sites of bedsores include:
- Lower back (sacral area).
- Heels.
- Hips.
- Elbows.
- Shoulder blades.
Patients at higher risk include elderly individuals, stroke survivors, spinal cord injury patients, postoperative cases, and those with reduced sensation, poor nutrition, or chronic conditions such as diabetes.
How Bedsores Hamper the Rehabilitation Process
Bedsores can become a major barrier in home rehabilitation if not identified and managed early.
They affect rehabilitation in several ways:
- Pain and discomfort, leading to poor participation in exercises.
- Restricted positioning, limiting bed mobility, sitting balance, and transfer training.
- Delayed progress in standing, walking, and functional independence.
- Increased risk of infection, sometimes requiring hospital readmission.
- Emotional distress, fear of movement, and reduced motivation.
Simply put, when a patient is uncomfortable or in pain due to bedsores, effective rehabilitation becomes extremely challenging.
Role of Home Rehabilitation in Preventing Bed Sores
A structured home rehabilitation program plays a key role in preventing pressure ulcers. Rehabilitation is not limited to exercises alone—it also focuses on movement, positioning, and education.
Preventive strategies include:
- Regular position changes, ideally every two hours.
- Training in bed mobility, such as rolling and repositioning.
- Maintaining correct sitting posture in bed and in a wheelchair.
- Using pressure-relieving cushions and mattresses.
- Educating caregivers about positioning, skin inspection, and daily movement.
Physiotherapists are trained to identify early signs of pressure damage and adapt rehabilitation plans to reduce risk.
Managing Bed Sores During Home Rehabilitation
If bedsores develop, rehabilitation should continue with appropriate modifications while prioritizing healing.
1. Positioning and Pressure Relief
- Avoid prolonged pressure on the affected area.
- Use pillows, wedges, and supports to offload pressure.
- Follow a consistent turning and repositioning schedule.
2. Exercise Modification
- Continue pain-free range of motion exercises.
- Focus on strengthening unaffected body parts.
- Gradually reintroduce functional activities without stressing the wound area.
3. Wound Care Support
- Maintain cleanliness and hygiene.
- Follow the wound care advice provided by doctors or nurses.
- Avoid self-treatment of advanced or infected bedsores.
4. Nutrition and Hydration
Nutrition plays a crucial role in wound healing.
- Adequate protein intake.
- Proper hydration.
- Vitamins and minerals as advised by healthcare professionals.
A Multidisciplinary Approach to Home Rehabilitation
Effective home rehabilitation requires collaboration between:
- Doctors.
- Nurses.
- Physiotherapists.
- Caregivers.
- Dieticians.
This team-based approach ensures proper wound healing, uninterrupted rehabilitation, and reduced complications, ultimately leading to better recovery outcomes.
A Physiotherapist’s Perspective
As a physiotherapist working in home rehabilitation, I frequently observe that bedsores are often underestimated in the early stages. Many patients and caregivers focus primarily on exercises or walking, while skin health is unintentionally neglected.
From a rehabilitation standpoint, bedsores are not just a skin issue—they directly affect posture, movement, and participation in therapy. Pain from pressure ulcers can restrict basic activities such as rolling in bed, sitting upright, or standing, all of which are fundamental components of home rehabilitation.
Early intervention makes a significant difference. Simple measures like timely repositioning, correct bed and wheelchair positioning, pressure relief techniques, and caregiver education can prevent most bedsores. Even when bedsores are present, rehabilitation does not stop—it adapts. Therapy is modified to promote healing while maintaining joint mobility, muscle strength, and functional independence.
In home-based care, educating caregivers is equally important. Teaching safe handling techniques, recognizing early warning signs of pressure damage, and incorporating movement into daily routines ensures continuity of care beyond therapy sessions.
Successful rehabilitation is achieved when comfort, dignity, and mobility are addressed together.
When to Seek Immediate Medical Attention
Patients and caregivers should seek medical help if they notice:
- Fever or signs of infection.
- Increasing redness, swelling, or pain.
- Foul-smelling discharge.
- A wound that is not healing or worsening.
Early medical intervention can prevent serious complications.
Conclusion
Home rehabilitation is more than just performing exercises—it is about holistic patient care. Bedsores can significantly delay recovery, but with timely prevention, appropriate management, and coordinated care, patients can continue rehabilitation safely and effectively.
By prioritizing skin integrity along with physical recovery, home rehabilitation programs can achieve faster progress, better outcomes, and improved quality of life.
Author
Mayuri Sabnis, MPT
Consultant Physiotherapist
(Home Rehabilitation Specialist)
