What Are Bedsores? Causes, Stages, Symptoms & Prevention
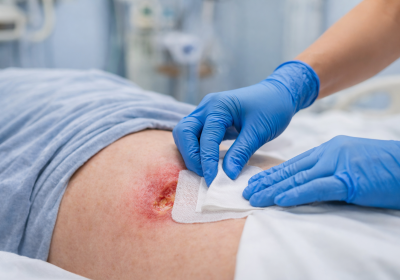
Bedsores—also known as pressure sores or pressure ulcers—are skin and tissue injuries that develop when prolonged pressure reduces blood flow to an area of the body. They most commonly affect people who are bedridden, wheelchair-bound, recovering from surgery, elderly, or living with diabetes or mobility limitations.
Without timely care, bedsores can worsen quickly—from mild redness to deep, infected wounds—impacting recovery, comfort, and overall quality of life.
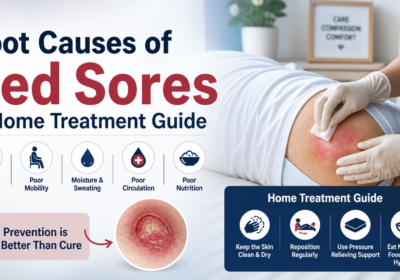
What Causes Bedsores?
Bedsores occur due to a combination of:
1. Prolonged Pressure
Continuous pressure over bony areas (hips, heels, tailbone, shoulders, and elbows) restricts blood circulation, starving tissues of oxygen and nutrients.
2. Friction
When skin rubs against clothing or bedding, it weakens the surface and increases vulnerability.
3. Shear
Sliding down in a bed or wheelchair causes the skin to move in one direction while underlying tissues move in another—damaging deeper layers.
4. Moisture
Excess moisture from sweat, urine, or wound discharge softens the skin, making it prone to breakdown.
Common Areas Where Bedsores Develop
- Lower back (sacrum).
- Hips.
- Heels.
- Ankles.
- Elbows.
- Back of the head.
- Shoulders.
- Inner knees.
These are pressure-prone areas, especially in patients who remain in one position for long periods.
Stages of Bedsores
Bedsores progress in stages depending on severity:
Stage 1 – Early Warning
- Redness or discoloration
- Skin feels warm or firm
- Pain or tenderness
- Skin remains intact
This stage is reversible with immediate intervention.
Stage 2 – Partial Skin Loss
- Open blister or shallow wound
- Pink or red base
- Mild swelling or drainage
Early wound care is crucial to prevent infection.
Stage 3 – Deep Wound
- Visible fat tissue
- Crater-like appearance
- Possible discharge or foul odor
Requires medical supervision and structured wound management.
Stage 4 – Severe Tissue Damage
- Deep wound exposing muscle, bone, or tendon
- High risk of infection
- Requires urgent medical care
Advanced ulcers can lead to serious complications if untreated.
Symptoms to Watch For
Early detection can prevent complications. Look for:
- Persistent redness or darkened patches.
- Swelling.
- Pain or burning sensation.
- Blisters or open wounds.
- Drainage or pus.
- Foul smell from the wound.
- Fever (in case of infection).
Caregivers should inspect vulnerable areas daily.
Who Is at High Risk?
- Bedridden or wheelchair-bound patients.
- Post-surgery patients.
- Elderly individuals.
- People with diabetes.
- Patients using diapers.
- Individuals with reduced sensation (nerve damage).
- Malnourished or dehydrated individuals.
How to Prevent Bedsores
Prevention is always better than treatment. Here’s how:
Reposition Frequently
Change position every 2 hours (bed) or every 15–30 minutes (wheelchair).
Maintain Skin Hygiene
Keep skin clean and dry. Use gentle cleansers and pat dry.
Use Support Surfaces
Air mattresses, pressure-relieving cushions, and soft padding reduce pressure.
Inspect Skin Daily
Check high-risk areas for redness or irritation.
Maintain Proper Nutrition
Protein, vitamins (especially C and Zinc), and hydration support skin repair.
Manage Moisture
Use protective barriers if incontinence is an issue.
When to See a Doctor?
Seek medical attention if:
- Redness doesn’t improve within 24–48 hours.
- The wound deepens or drains pus.
- Fever develops.
- The patient experiences increasing pain.
Early professional care prevents serious complications.
Final Thoughts
Bedsores are preventable—but only with awareness and consistent care. Whether caring for a loved one at home or managing patients in a healthcare setting, early detection and timely intervention make a significant difference.
If you or someone you care for is at risk, adopt a structured skin care and repositioning routine immediately. Small preventive steps today can avoid serious health challenges tomorrow.